Multiple sclerosis (MS) is a highly heterogeneous disease. Patients respond differently to medications and have disease prognoses that vary greatly. The new Clinical Research Priority Program (CRPP) PrecisionMS looks at how therapies can be adapted to the individual patients’ disease. We talked with Prof. Roland Martin, head of the CRPP about the goals of the program.

ZNZ News: What is the aim of the CRPP precision MS?
Prof. Roland Martin: Multiple sclerosis is an autoimmune disease that damages the brain and spinal cord and in which both environmental and genetic factors play a role. The interplay between these factors leads to the large degree of heterogeneity: Patients can have completely different disease courses and a wide range of neurological signs and symptoms and, for example, different imaging findings. Finally, the responsiveness to treatment varies between patients as well. In this new program, we want to assess the individual patient’s disease as best and early as possible to determine how closely a patient needs to be followed and to adjust the treatment.
How does the focus of the CRPP differ from the previous Multiple Sclerosis CRPP?
In the previous CRPP we embarked on dissecting the heterogeneity with a relatively broad set of approaches: Several groups were working on MR imaging of the brain and spinal cord, others on imaging of the eye or electrophysiological techniques, and several were using immunological or neuropathological techniques both in animals and in humans to identify disease subtypes and identify imaging- or biomarkers. Another important goal was to set up the infrastructure for clinical trials to conduct first experimental, investigator-initiated trials. Now, we want to bring our knowledge to the clinic to characterize patients with respect to their individual risk and adjust treatment accordingly and much more precisely.
What is your vision for future treatment of MS patients?
Our bold goal is to cure MS, meaning that we have treatments that are so effective that we can stop the disease completely in a large fraction of patients. The transplantation of autologous hematopoietic stem cells is probably closest to that goal right now. We have received approval from the Swiss health authorities to perform this treatment here in Zurich for entire Switzerland. It is, however, an intense treatment with potentially severe side effects and thus not the best option for many patients. In the future, we need to develop treatments that are equally effective but less invasive. Therefore, we have developed a treatment to induce immune tolerance with peptide-coupled red blood cells in MS patients (by A. Lutterotti, R. Martin and his team, also supported by the Wyss Zurich). With the phase I clinical trial successfully closed, the project will continue under the CRPP PrecisionMS. Another vision is to combine treatments that stop the disease by inhibiting the immune system with treatments that protect cells of the nervous system and myelin, or even repair them, so we can reverse already existing damage.
What is needed to make this vision come true?
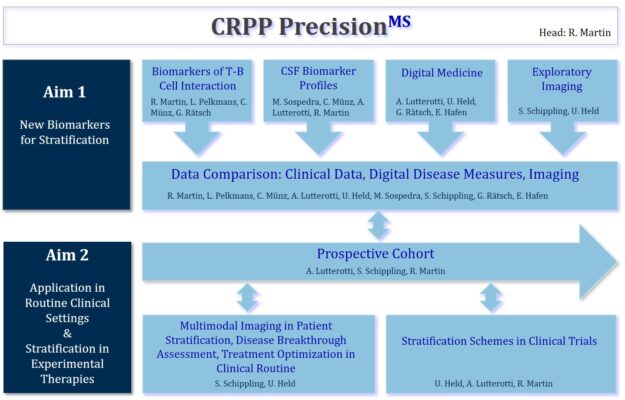
A key requirement is a collaborative approach by combining the expertise of several research groups. The spectrum ranges from basic experiments in vitro in the laboratory (Mireia Sospedra, Christian Muenz, Lukas Pelkmans, University of Zurich & University Hospital Zurich) to translating and evaluating novel parameters for stratification and treatment response in patient care (Ernst Hafen, Gunnar Rätsch ETHZ, Ulrike Held, University of Zurich) and testing novel treatments in patients (Roland Martin, Sven Schippling, Andreas Lutterotti).
Important topics @ the CRPP PrecisionMS
Biomarkers of T-B Cell interaction